
In summary, late lead perforation should be considered if patients present with chest pain and pacemaker malfunction. Unfortunately, it remains speculative if the unusual QRS vector was an expression of anodal stimulation because no 12-lead surface ECG with effective ventricular stimulation was documented before the patient was referred to our institution. 5b) excluded a left ventricular position of the pacing lead. 
This observation suggests left ventricular stimulation, but the lateral chest X-ray (Fig. 3), the precordial leads showed a right bundle branch block-like deformed QRS complex. In the ECG that was taken during ‘bipolar’ stimulation with the perforated lead (Fig. This observation suggests anodal stimulation from the RV lead ring, because CT scan illustrated that the perforated electrode tip was outside the myocardium and tip-ring spacing of Medtronic 4074 lead is 17 mm. In our case, efficient pacing could at least transiently be achieved with the perforated lead by changing the pacing polarity from unipolar to bipolar. Several risk factors for lead perforation with symptomatic pericardial effusion after permanent pacemaker implantation are discussed: use of a temporary transvenous pacemaker, steroid use within 7 days prior to implant, use of helical screw ventricular leads, older age, body mass index <20 and longer fluoroscopy times. Multidetector CT has been shown to be a useful tool for verifying the diagnosis. Ĭonventional chest X-ray and transthoracic echocardiography can be helpful in diagnosis but occasionally fail to identify lead perforation. On the other hand, completely asymptomatic cases of late lead perforation have also been described. Rare cases of cardiac tamponade or death have been documented in patients with late lead perforations. Less frequently, late lead perforation may cause chest pain, hemopneumothorax and pneumothorax. Most commonly, this complication manifests with pacemaker malfunction such as insufficient cardiac stimulation and resulting symptoms such as dizziness (as in our case) or syncope. Symptoms of late lead perforation are commonly subtle and unspecific. Rare cases of lead perforation later than 1 year have been reported. Delayed lead perforation (≥1 month after implantation) occurs in 0.1–0.8% of pacemaker implantations. Acute perforation of the right ventricle has been reported in up to 1% of patients and is normally associated with haemorrhagic pericardial effusion and haemodynamic instability due to tamponade, necessitating pericardial drainage and occasionally surgical intervention. Lead perforation is a rare complication in patients undergoing pacemaker implantation. Postoperative device interrogation demonstrated a stable unipolar pacing threshold of 0.5 V at 0.5 ms. The lead could be removed without complications and a new RV lead (same model, 4074 CapSure Sense, Medtronic, USA) was implanted in the lower RV close to the apex. Based on these findings, elective lead extraction was performed in the operating theatre with backup for emergency thoracotomy because of the elevated procedural risk for haemorrhagic pericardial effusion and tamponade. CT imaging and echocardiography excluded significant pericardial effusion. This diagnosis was confirmed by native multidetector computed tomography (CT) of the chest (Fig. 5a) was found to be suggestive for late lead perforation. 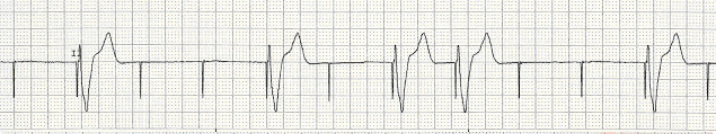
In our case, no conclusions could be drawn from the post-implant X-ray due to a low image quality, but in consideration of the patient history, the current chest X-ray (Fig. In this situation, the comparison of a current chest X-ray with the image taken earlier after implantation may verify lead dislocation. 
We found excellent sensing parameters, an inconspicuous pacing impedance, unipolar exit block and bipolar capture with an elevated pacing threshold. In our case, device interrogation revealed dubious findings. In patients with presumed pacemaker dysfunction, device interrogation should be performed first.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
